Contents:
- Introduction
- Diagnosis and pre-op
- Talking to your healthcare team
- What is a urostomy?
- How long does it take to recover after urostomy surgery?
- How should a stoma look?
- What are the likely changes to daily life after surgery?
- What pouches are available?
- Emotional effects of having a urostomy
- Taking good care of yourself
- Support for carers
Introduction
Most people who have surgery for a urinary diversion find they recover well and can maintain their independence; but this is not always straightforward or possible. They may need their partner, friend or family member to be their caregiver in the short term as they adjust to their new way of living. And, in the longer term, they may need support and understanding as they learn to live life to the full again.
If you are caring for your loved one, it can feel rewarding knowing you are playing a big part in helping them stay as well and as active as possible. However, it can sometimes be demanding both physically and emotionally, especially if you are juggling your caring responsibilities with work and other activities.
It is natural to have times when you feel sad, anxious or angry, but please remember that you are not alone. There are many forms of support, both online and in your local community – sometimes it is just a case of knowing where to look for help.
The Urostomy Association is here for you for as long as you need us.
As well as covering basic information about urostomies and addressing common concerns, this page includes tips on providing emotional support for your loved one and communicating with their healthcare team. There’s also advice to help you take good care of yourself too.
Diagnosis and pre-op
Being told that your loved one needs a urinary diversion can be daunting for both of you, and the best way to overcome your fears and prepare for the future is to ask lots of questions from those in the know.
But, before that, take a big breath and approach the next few weeks as calmly as you can. You may feel that you need to be the strong one, but you don’t have to carry this responsibility alone.
You can contact our helpdesk, download resources from this website or ask us to put you in touch with one of our friendly, trained volunteers who can provide support over the telephone or in person. You’ll find our contact details here and, at the bottom of this page, you can find details of other organisations providing information and support for carers.
We have been talking to urostomates and those who care for them, face-to-face, through our helpline and our private Facebook group, to compile the ten frequently asked questions. These appear on our diagnosis and pre-op page.
You are likely to want to keep family, friends and children appropriately informed. Our Bags, Bags, Bags book can help you explain the situation to young children, but adult children will also want information and support and they may well turn to you for that. You may have to respond to questions such as ‘Will they die?’, ‘Is it hereditary?’, ‘Can I still cuddle them?’
Remember to keep friends informed too, and often this will involve you helping to send emails and answer telephone calls if they become too much for your loved one to manage alone. This keeping people informed is especially important during operations or after a difficult diagnosis.
Talking to your healthcare team
You are an important part of the care team looking after your loved one, and educating yourself about their condition can help ease some of anxiety associated with stoma surgery and how life may be afterwards.
Try to accompany your loved one on their stoma nurse appointments, and compile between you, in advance, what questions you’d like to ask. Try and remember to write down the answers as you’re likely to feel a little overwhelmed to start with, and may find it difficult to hold all the information in your head.
If you don’t understand something, ask the stoma nurse to explain it further or to draw a picture. If you have a lot of things to talk about, it’s a good idea to ask for a consultation appointment so there’s more time for discussion.
While the nurse can teach you skills so that you can help your loved one manage their stoma at home, do encourage them to do as much of their own care as possible. This will help them maintain their sense of independence and gain confidence. Be open to new ideas, and don’t hesitate to seek help when you need it.
What is a urostomy?
A urostomy is an opening (stoma) on the abdomen made during surgery. It lets urine drain out of the body from the kidneys if the bladder has been removed.
The procedure is typically necessary when there is a problem with the normal urinary system and urine can’t be released through the usual route (through the urethra). Common reasons why someone might need a urostomy include bladder cancer; conditions affecting the nerves controlling the bladder, such as multiple sclerosis or spinal cord injuries; congenital abnormalities; chronic infections or fistulas, and severe interstitial cystitis.
- You can find more detail on our ‘What is a urostomy’ page
How long does it take to recover after urostomy surgery?
Recovery time can vary from person to person and depends on several factors, including overall health, the reason for the urostomy, the type of operation (open or robotic), and any complications that may arise. The good news is that most people are able to resume normal activities within a few weeks to a couple of months after their operation.
How should a stoma look?
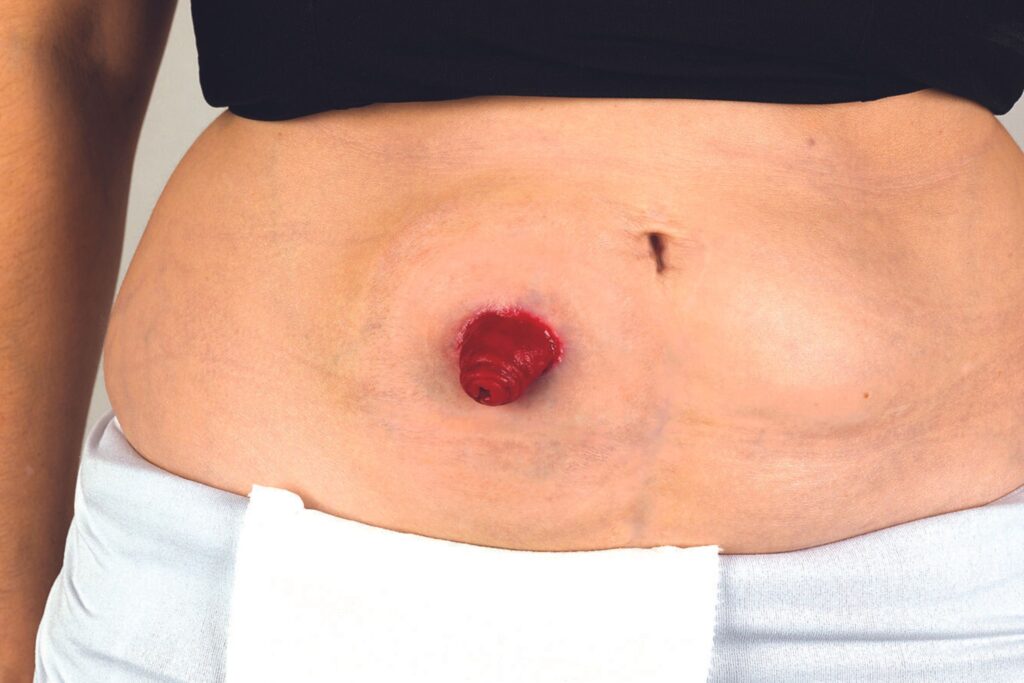
A healthy stoma, like the one shown here, is moist and red, similar to the inside of your mouth. It will probably be swollen after surgery and can take several weeks or months to shrink to its permanent size.
What are the likely changes to daily life after surgery?
For most new urostomates, life can feel challenging initially, but with time and support they become more confident about living with their stoma. The specialist nurse will give advice about stoma care at home. They can also help arrange supplies of equipment. Talk to them if you have any questions or experience any problems.
Caring for a stoma: As there are no nerve endings, your loved one shouldn’t experience any pain or discomfort from their stoma itself. However, it will require regular care to keep it clean and healthy. This involves changing the urostomy bag and cleaning the area of the stoma. Learning how to properly apply and change the bag is an important aspect of post-urostomy life. During your loved one’s hospital stay they will be shown how to do this.
Diet and hydration: Great news – having a urostomy won’t mean that your loved one has to give up their favourite food and drink. What’s really important is staying well hydrated. As well as being vital for kidney health and helping to prevent urinary tract infections (UTIs), drinking enough water – six to eight glasses a day – can also prevent urine from becoming too concentrated and causing skin irritation or discomfort around the stoma.
Physical activity: Having a stoma shouldn’t be a barrier to being active. From easily handling everyday chores to getting back into exercise, there are very few restrictions. However, it takes time to heal after stoma surgery, and your loved one’s consultant or stoma nurse will be able to advise on returning to normal activities.
Parastomal hernias: A parastomal hernia can be a common occurrence and can happen at any time. It is a term used to describe a bulge or swelling around or under the stoma that can lead to problems with stoma. It is important, in the early days post operation, that the patient takes things easy, allowing time for the muscles in the abdominal wall to regain strength. The length of time varies from person to person and whether the operation has been done through open surgery or robotic. The latter generally involves less recovery time.
Clothing: Having a stoma doesn’t mean having to change personal style and invest in a whole new wardrobe. Stretchy clothes are a good idea for straight after surgery, but once fully healed, there’s nothing to stop your loved one from wearing any clothes that make them look and feel good.
However, there are brands providing all types of clothing specifically for ostomates, from swimwear and underwear to casual clothing.
- See our ‘Directory of suppliers’ page for examples of speciality clothing retailers.
Sex and intimacy: Recovering from stoma surgery may temporarily put your sex life on hold, but there’s no reason you can’t resume intimacy when the time feels right. Try to have honest and open talks with your partner about expectations for resuming your sex life. Your partner might be feeling anxious about how you will react to their body. Talking to them can help reduce that worry.
Travel: From organising a day out to holidaying abroad, travelling may require additional planning, especially in terms of carrying extra supplies and understanding how to manage the urostomy in different environments.
- Our Travelling with confidence page contains more useful information. You may also like to watch Donna Watson’s ‘A tale of two holidays’ video in which she describes her first short break after her urostomy and then, once she’d got her confidence, her exploits much further afield.
You may like to see the ‘Understanding issues which may arise with a urinary diversion’ page for more on what to expect following surgery.
What pouches are available?
There are a wide variety of urostomy pouches available, made by several manufacturers. Pouches are waterproof and odour-proof and have skin-friendly adhesives, which act as a protective barrier for the skin around the stoma. The pouches are fitted with a non-return valve, which prevents the urine in the pouch from flowing back over the stoma. The pouches all have a tap or bung at the bottom, which allows for emptying into the toilet when the pouch is becoming full, leaving the pouch in place to continue collecting wee.
Pouches are available as either one-piece or two-piece products.
Two-piece systems consist of an adhesive flange, which is stuck to the skin around the stoma, and a pouch attached onto the flange to collect wee. With this type of pouch, the flange can typically remain on the abdomen for three to five days, with only a need to change the pouch.
One-piece systems consist of a pouch with the adhesive flange sealed directly onto it, which means that the whole pouch needs to be changed each time. Typically, these can be left on the skin for one to three days before the pouch needs to be changed.
Both types are available in a range of pre-cut sizes or with a starter hole that can be cut to fit individual stomas. You might find that the pre-cutting option is very useful once the stoma has retained a regular shape, especially if you have sight or dexterity issues which can make cutting the pouches difficult.
The pouch changes we recommend here are only guidelines and your loved one’s stoma care nurse will be able to provide personalised advice. Urostomy pouches and other items essential for care of the stoma are available on prescription without charge. An exemption form will need to be completed for anyone aged under 60.
Emotional effects of having a urostomy
When someone is told they need to have a urinary diversion and will need to wee differently for the rest of their life, it can feel overwhelming and difficult for them to imagine what lies ahead.
Feelings of fear, sadness and anger are common responses to dealing with a diagnosis and stoma surgery, and you may need to help your loved one cope with all these emotions.
Sometimes a person may direct their emotions toward their caregiver. Naturally, this may be upsetting for you but try to remember that people often displace their feelings onto those closest to them because you feel like a ‘safe outlet’.
Here are some tips that may help you provide emotional support:
- Being together and listening are the most important parts of caring and comforting your loved one
- Encourage them to open up about their concerns
- Let them know it’s okay to feel sad as they learn how to adjust to their new way of living
- Practice positive coping skills together, such as relaxation techniques
- Plan activities you can enjoy together, like visiting friends and family, watching a favourite TV programme or going for a walk. These help to remind you that life can continue as normal, and will help you to take your mind off things for a while
- Find a local support group where you can meet with others in similar circumstances for mutual support
- Respect your loved one’s need for space but remind them you are there if they want to talk
- Be ready to listen to what your loved one wants and to give support, but try not to overly challenge them if you don’t agree with their approach.
Taking good care of yourself
When you spend a lot of your time focusing on someone else, you may feel as if you have no time for yourself. But looking after your own wellbeing is important for you and for them. Remember to be gentle on yourself when things feel stressful. By caring for yourself, you will be better able to care for your loved one.
Tips for self-care:
- Share your feelings with someone you trust, such as a friend or family member
- Look after your physical health by eating as healthily as you can and getting some form of regular exercise
- Ask for help if you need it and be as specific as possible about what others can do to ease some of the pressure on you
- Take breaks and try to make time for things you enjoy, such as a relaxing bath, coffee with a friend or watching a film
- Try to get enough sleep as a lack can make it harder to cope with everyday challenges
- Do confide in a healthcare professional, such as your GP or a counsellor, if it would help to talk about your feelings.
If you are finding it hard to balance caring with paid employment, you have a right to ask your employer about flexible working arrangements. To make this request you need to have worked for the same employer for at least 26 weeks. Your flexible working request could involve going part time, changing your work pattern or job sharing. You are also entitled to reasonable time off work to deal with emergencies.
Support for carers
At the Urostomy Association, we can put you in touch with other people who are caring for a urostomate, so you can talk to someone who can understand, first hand, your queries and concerns. Please remember that our charity is here for you and your loved one with information, support and advice to help you both stay well so you can enjoy life. We’re here for as long as you need us.
Listed below are also some other sources of support you may find useful.
Citizens Advice
Free, confidential information and advice on your rights, including money, housing, experiences of discrimination and other problems
0800 144 8848 (England Adviceline)
0800 702 2020 (Wales Adviceline)
18001 0800 144 8884 (textphone)
citizensadvice.org.uk
Carers Trust
Information and support for people caring for someone else
0300 772 9600 (Mon – Fri, 9am – 5pm)
carers.org
Carers UK
Advice and support for anyone who provides care
0808 808 7777
029 2081 1370 (Carers Wales)
advice@carersuk.org
carersuk.org
Mind
Mental health advice and support
0300 123 3393
info@mind.org.uk
mind.org.uk
Turn2us
Helping people in financial difficulty to access benefits, grants and support services.
turn2us.org.uk



