This information is for anyone who has, or is about to have, a urostomy. It explains what a urostomy is and why it may be necessary.
Once our bodies have absorbed as much as possible from the food or liquid we eat and drink, anything remaining that it cannot use is either absorbed into the bloodstream or passed through the bowel, as waste.
Waste in the bloodstream is filtered out in the kidneys and made into urine. Usually, our urine passes from our kidneys down a tube called the ureter; each kidney has a ureter that feeds into the bladder.
Our urine is stored in our bladders until they become full and we feel the need to go for a wee. When we go for a wee, our urine drains from the bladder via a single tube called the urethra. If a problem is encountered that disrupts our urine flow, it may be necessary to create a new exit so our wee can be passed out of our bodies. This may be due to the bladder or urethra becoming diseased or not working efficiently.
A urostomy (also referred to as an ‘ileal conduit’) is the creation of a new exit for our urine to leave the body via a stoma.
Forming the stoma
The word ‘stoma’ comes from the Greek language and means ‘mouth’. A stoma is an artificial opening on the surface of the abdomen. In the case of a urostomy, it is to allow urine to exit our bodies. During surgery, a piece of small bowel, about 10cm long, is removed. The two ends of the remaining small bowel, from where the piece has been removed, are joined together so our bowels can continue to function.
Once the piece of bowel has been removed, the ureters from each kidney are disconnected from the bladder and stitched to the outer surface, thus creating an exit from the body. This is the stoma. We then need to wear a urostomy pouch over the stoma at all times to collect the wee as it leaves our bodies. During the operation, to assist the healing process, fine tubes, called ‘stents’, are inserted into the kidneys, via the ureters, so our kidneys can more freely be drained of wee. These stents either fall out or are removed roughly ten days after surgery.
Why is a urostomy necessary?
There are a variety of reasons why we might need a urostomy, but it is usually because of a defect or problem within the lower urinary system, which needs to be removed or bypassed. Examples include:
- Bladder or pelvic cancer
- Birth defects such as Spina Bifida, Cerebral Palsy or a malformation within the urinary system
- Trauma to the spine or gynaecological problems.
Some people may also choose a urostomy for social reasons because it is easier to manage than a defective bladder. With this condition, patients struggle to control the flow of urine, causing them embarrassment and problems with their skin, due to it being constantly wet.
The stoma
A healthy stoma is moist and red, similar to the inside of your mouth. As your small bowel produces mucus to ease the passage of waste food through it, it will continue to do so. So the piece of small bowel that has been used to form your stoma will continue to produce mucus which will mix with your wee in the pouch.
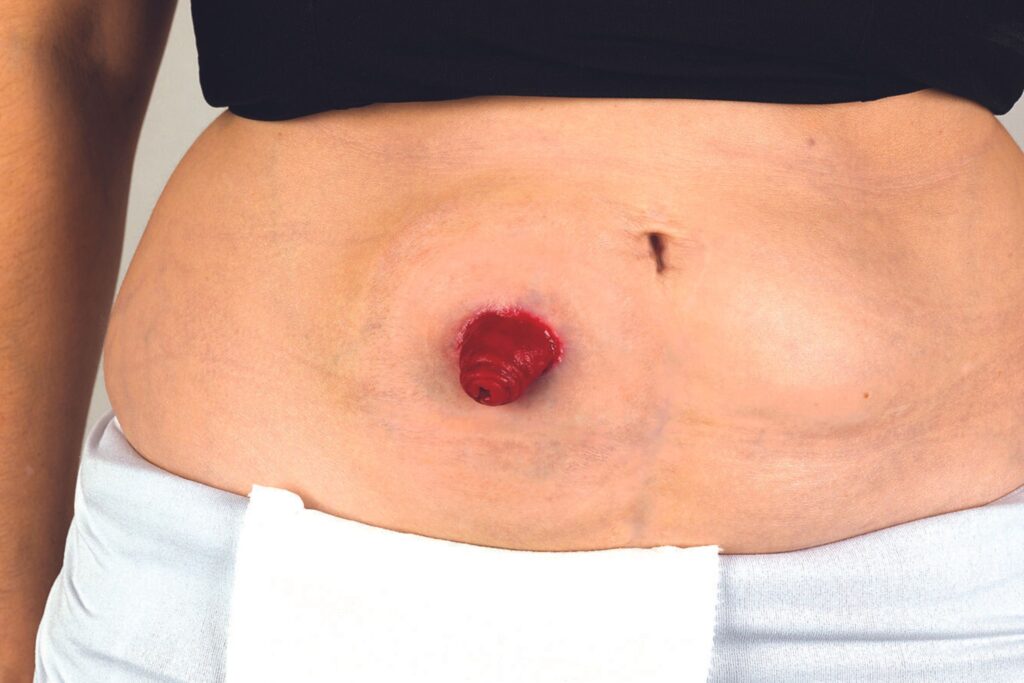
Mucus is visible in your wee as a whitish, jelly-like substance. This is quite normal and may decrease in time. As the stoma does not have nerve endings, it has little sensation and isn’t painful when touched. However there is a rich blood supply close to the surface, and you may find that your stoma bleeds sometimes when you clean it. This shouldn’t be a cause concern, but reminds you to handle your stoma with care.
Sometimes the stoma can be seen to move – this is the normal movement of the bowel (known as peristalsis), and helps to direct the urine outwards into the urostomy pouch.
Urostomy pouches
There are a wide variety of urostomy pouches available, made by several manufacturers. Pouches are waterproof and odour-proof and have skin-friendly adhesives, which can act as a protective barrier for the skin around your stoma.

The pouches are fitted with a non-return valve, which prevents the urine in the pouch from flowing back over the stoma. The pouches all have a tap or bung at the bottom, which allows you to empty it into the toilet when the pouch is becoming full, leaving the pouch in place to continue collecting your wee.
Different types of urostomy pouches
Pouches are available as either one-piece or two-piece products. Two-piece systems consist of an adhesive flange, which is stuck to the skin around the stoma, and a pouch attached onto the flange to collect your wee. With this type of pouch the flange can typically remain on your abdomen for three to five days, with only a need to change the pouch.
One piece systems consist of a pouch with the adhesive flange sealed directly onto it, which means that you change the whole pouch each time. Typically these can be left on the skin for one to three days before the pouch needs changing. Both types are available in a range of pre-cut sizes or with a starter hole that can be cut to fit individual stomas. You might find that the pre-cutting option is very useful once your stoma has retained a regular shape, especially if you have sight or dexterity issues which can make cutting the pouches difficult.
The pouch changes we recommend here are only guidelines and your stoma care nurse will advise be able to advise you personally.
Urostomy pouches and other items essential for care of the stoma are available on prescription without charge. If you’re under 60, you will need to complete an exemption form.
Do you want to speak to someone?
From talking to people who have had surgery, we find that many are able to return to an active or rewarding lifestyle after surgery and we often hear people describe it as ‘restoring their quality of life’. There are some inspirational stories from urostomates on our blog page; do take a look.
If you’d like to speak to a Urostomy Association volunteer buddy with personal experience of a urinary diversion, please contact the office and we’ll put you in touch.
* The photos of the stoma and urostomy bags are courtesy of Hollister Ltd
The information on this page is available as a downloadable leaflet.




